Endometriosis Treatment in Delhi – Advanced Laparoscopic & Multidisciplinary Care
Endometriosis is a chronic and often misdiagnosed condition that affects women of reproductive age, leading to severe pelvic pain, infertility, and reduced quality of life. If you are looking for the best endometriosis treatment in Delhi, expert endometriosis specialists, or laparoscopic endometriosis surgery in Delhi, Sunrise Hospital offers comprehensive, world-class care under one roof.
Our Endometriosis Centre of Excellence in South Delhi provides advanced diagnosis, minimally invasive laparoscopic surgery, fertility-focused treatment, and long-term pain management through a multidisciplinary team of gynecologists, laparoscopic surgeons, fertility experts, bowel surgeons, urologists, radiologists, and pain specialists.
What is Endometriosis?
Endometriosis is a medical condition in which tissue similar to the endometrium grows outside the uterus. Unlike normal endometrial tissue that sheds during menstruation, this tissue can attach to other organs and create inflammation, scar tissue, and adhesions, often causing severe pain and organ dysfunction. The most commonly affected areas include:
- Ovaries – Can lead to cysts known as endometriomas.
- Peritoneum – Causes adhesions that make organs stick together.
- Intestines and rectum – Leading to bowel pain, constipation, or diarrhea.
- Urinary system – Involving the bladder and ureters, causing painful urination.
- Rarely – Nerves and lungs, causing nerve pain or breathing difficulties during menstruation.
Types of Endometriosis We Treat
- Superficial peritoneal endometriosis – Small lesions on the peritoneum.
- Ovarian endometriosis – Formation of endometriotic cysts in the ovaries.
- Deep infiltrating endometriosis (DIE) – Tissue penetrating organs like the bowel or bladder, requiring complex surgery.
- Extrapelvic endometriosis – Rare involvement of lungs, diaphragm, or nerves.
Common Symptoms of Endometriosis
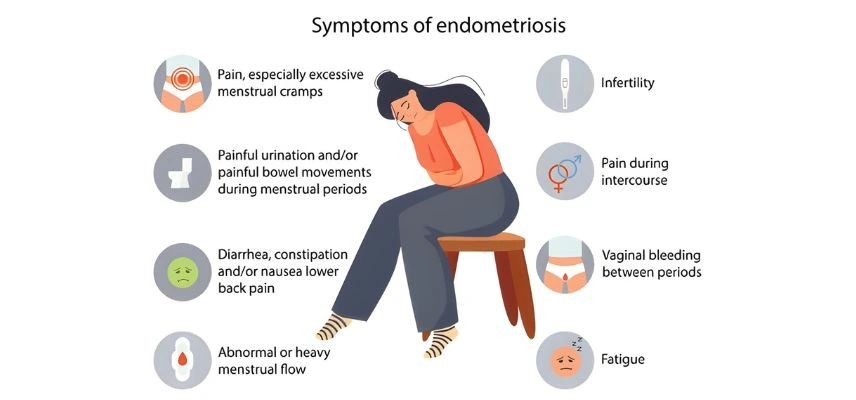
Women experiencing pelvic pain, painful periods, infertility, bowel or urinary symptoms should consult an endometriosis specialist in Delhi for early diagnosis.
Endometriosis presents with a variety of symptoms, which can range from mild to debilitating. Understanding these symptoms is crucial for early detection and effective treatment.
Pain During Menstruation (Dysmenorrhea)
One of the most common symptoms, dysmenorrhea refers to severe cramping and pelvic pain during menstruation. Women may also experience lower back pain and abdominal discomfort, often affecting daily activities.
Pain During Intercourse (Dyspareunia)
Endometriosis can lead to deep pelvic pain during or after sexual intercourse, significantly affecting intimate relationships and quality of life.
Infertility and Fertility Challenges
Endometriosis is a leading cause of infertility. Scarring, adhesions, and ovarian cysts can interfere with egg release and fertilization. Couples may require IVF or other assisted reproductive techniques.
Painful Bowel Movements and Constipation (Dyschezia)
Endometrial lesions affecting the bowel can cause painful defecation, bloating, constipation, or diarrhea, often worsening during menstruation.
Pain During Urination (Dysuria)
Endometriosis can involve the bladder or ureters, leading to pain, frequency, or burning sensation during urination.
Rare Symptoms
In severe cases, endometriosis can affect nerves or the lungs, causing nerve pain (especially in the sciatic nerve region), coughing up blood during menstruation, or breathlessness.
Causes and Risk Factors of Endometriosis
While the exact cause of endometriosis remains unclear, several theories and risk factors have been identified:
- Retrograde Menstruation: Menstrual blood flows backward through the fallopian tubes into the pelvic cavity.
- Hormonal Imbalance: High levels of estrogen can promote endometrial tissue growth outside the uterus.
- Genetic Predisposition: Family history increases susceptibility.
- Immune System Dysfunction: Impaired immune response may prevent the body from removing abnormal tissue.
- Surgical Scars: Rarely, endometrial tissue may implant at surgical incision sites.
Diagnosis of Endometriosis
Early and accurate diagnosis is vital for effective treatment. At Sunrise Hospital, endometriosis evaluation is conducted by a multidisciplinary team of experts.
Sunrise Hospital follows international diagnostic protocols for accurate detection of deep endometriosis, bowel endometriosis, and bladder involvement.
Clinical Evaluation
The process begins with a detailed history and physical examination. Symptoms, menstrual patterns, and reproductive health are carefully documented.
Imaging Studies
- Transvaginal Ultrasound: Detects ovarian endometriomas and deep infiltrating endometriosis.
- Rectal Saline Contrast Ultrasound: Helps assess bowel involvement.
- MRI / CT Scan: Recommended in complex or rare cases, such as lung or nerve involvement.
Multidisciplinary Assessment
A team comprising gynecologists, radiologists, colorectal surgeons, urologists, and pain specialists evaluates the patient to develop a personalized treatment plan.
Treatment Options for Endometriosis
Treatment at Sunrise Hospital is tailored to each patient based on the severity of symptoms, extent of disease, fertility goals, and overall health.
Medical Management / Hormonal Therapy
Hormonal therapy helps manage symptoms in early-stage endometriosis but may not cure advanced disease. Hormonal medications can reduce pain, slow disease progression, and manage symptoms. Common treatments include:
- Oral contraceptives
- Progestins
- Gonadotropin-releasing hormone (GnRH) agonists
- Anti-inflammatory medications
Laparoscopic Surgery (Minimally Invasive)
Laparoscopic surgery for endometriosis is the gold standard treatment for advanced disease, offering precise removal of lesions while preserving fertility. Surgery is often required for advanced endometriosis or when fertility is affected. Laparoscopic surgery offers:
- Complete removal of visible endometriosis
- Treatment of ovarian cysts and adhesions
- Minimal recovery time compared to open surgery
- Preservation of fertility wherever possible
The surgical team includes gynecologists, colorectal surgeons, and urologists working under guidance from anesthetists and pain management experts. Postoperative care follows AAGL (American Association of Gynecologic Laparoscopists) guidelines, providing patients with detailed visual and written surgical reports.
Multidisciplinary Surgical Approach
Endometriosis often affects multiple organs. A multidisciplinary approach ensures safe, comprehensive treatment. Specialists involved include:
- Gynecologic Laparoscopic Surgeons: Dr. Nikita Trehan & Dr. Hafeez Rahman
- Colorectal Surgeons: Dr. Rakesh Kumar & Dr. Sanjay Verma
- Urologists: Dr. Abhiyuttan & Dr. Saurabh Sinha
- Radiologists: Dr. Beena Tiwari
- Pain Management & Anesthesia: Dr. Mansi Dewan
- Clinical Psychologists: Dr. Bhavna Barmi
This multidisciplinary approach to endometriosis surgery in Delhi ensures complete disease clearance and long-term relief.
IVF & Fertility Treatments
Sunrise Hospital offers IVF treatment for endometriosis-related infertility, guided by experienced fertility specialists and embryologists. Women with endometriosis-related infertility are guided through IVF by expert consultants:
- Dr. Nidhi Jha & Dr. Pooja Garg
- In-house embryologist: Mr. Vikas Gautam
Psychological support is provided throughout to address emotional stress related to infertility.
Why Choose Sunrise Hospital for Endometriosis Treatment?
Sunrise Hospital stands out as a premier endometriosis center in Delhi due to:
- Multidisciplinary Expertise: Comprehensive evaluation by gynecologists, surgeons, radiologists, anesthetists, and psychologists.
- Advanced Technology: Latest imaging, minimally invasive surgery, and modern pain management techniques.
- Personalized Care: Individualized treatment plans based on patient needs and fertility goals.
- Centre of Excellence: Recognized for quality care, patient satisfaction, and clinical outcomes.
- Patient Support: Psychological counseling, pre- and post-operative guidance, and continuous follow-up.
- One of the best hospitals for endometriosis treatment in Delhi NCR
- Expertise in deep infiltrating and complex endometriosis surgery
- Fertility-preserving surgical techniques
Meet Our Expert Team
- Dr. Nikita Trehan & Dr. Hafeez Rahman – World-renowned gynecologic laparoscopic surgeons
- Dr. Nidhi Jha & Dr. Pooja Garg – IVF consultants
- Mr. Vikas Gautam – Full-time embryologist
- Dr. Rakesh Kumar & Dr. Sanjay Verma – Minimally invasive bowel surgeons
- Dr. Abhiyuttan & Dr. Saurabh Sinha – Urologists
- Dr. Beena Tiwari – Radiologist specializing in endometriosis
- Dr. Mansi Dewan – Pain management & anesthesia expert
- Dr. Bhavna Barmi – Clinical psychologist
Contact Sunrise Hospital for the Best Endometriosis Care in Delhi
Early consultation is crucial for managing endometriosis effectively. Sunrise Hospital provides world-class care with the best endometriosis specialists in Delhi. Book an appointment to access:
- Advanced diagnostic imaging
- Minimally invasive laparoscopic surgery
- Comprehensive IVF and fertility support
- Multidisciplinary pain management
- Expert guidance for long-term management and follow-up
Call us today or visit Sunrise Hospital, South Delhi, and get the best endometriosis treatment in Delhi from a team dedicated to restoring health, fertility, and quality of life.
Conclusion
Endometriosis is a challenging condition that requires early diagnosis, expert care, and a multidisciplinary treatment approach. Sunrise Hospital is a trusted destination for endometriosis treatment in Delhi, providing comprehensive care that combines advanced laparoscopic surgery, fertility management, hormonal therapy, pain relief, and psychological support.
Our mission is to enhance the quality of life for patients with endometriosis, help them achieve fertility goals, and provide relief from chronic pain. With our team of experienced specialists and cutting-edge technology, patients can access world-class endometriosis treatment in a safe and compassionate environment.
Take the first step towards better health and fertility. Consult the best endometriosis specialists at Sunrise Hospital today.
Frequently Asked Questions (FAQs)
Q1. What is the best treatment for endometriosis?
The best treatment depends on disease severity and fertility goals. Mild cases respond to hormonal therapy, while advanced cases require laparoscopic endometriosis surgery.
Q2. Who is the best endometriosis specialist in Delhi?
Sunrise Hospital has a dedicated Endometriosis Centre of Excellence led by expert laparoscopic gynecologists and multidisciplinary specialists.
Q3. Can endometriosis be cured permanently?
Endometriosis can be effectively managed. Complete laparoscopic excision surgery offers long-term relief in most patients.
Q4. Does endometriosis cause infertility?
Yes. Endometriosis is a leading cause of infertility. Surgical treatment and IVF for endometriosis patients can significantly improve pregnancy chances.
Q5. How long is recovery after laparoscopic endometriosis surgery?
Most patients recover within 1–3 weeks, depending on the complexity of surgery.