What Is Cervical Cancer?
Cervical cancer occurs when abnormal cells on the cervix grow out of control. The cervix is the lower part of the uterus that opens into the vagina. Cervical cancer specialist in Delhi can often be successfully treated when it’s found early. It is usually found at a very early stage through a Pap test.
What Causes Cervical Cancer?
Most cervical cancer is caused by a virus called human papillomavirus, or HPV. You can get HPV by having sexual contact with someone who has it. There are many types of HPV virus. Not all types of HPV cause cervical cancer. Some of them cause genital warts, but other types may not cause any symptoms. Get the Affordable and one of the best treatment of cervical cancer by Cervical Cancer Specialist in Delhi. So If you are looking for treatment, Visit us.
You can have HPV for years and not know it. It stays in your body and can lead to cervical cancer years after you were infected. This is why it is important for you to have regular Pap tests. A Pap test can find changes in cervical cells before they turn into cancer. If you treat these cell changes, you may prevent cervical cancer by Cervical cancer Treatment in Delhi. Consult with Cervical Cancer Doctor in Delhi.
What Are The Symptoms?
Abnormal cervical cell changes rarely cause symptoms. But you may have symptoms if those cell changes grow into cervical cancer. Symptoms of cervical cancer may include:
- Bleeding from the vagina that is not normal, or a change in your menstrual cycle that you can’t explain.
- Bleeding when something comes in contact with your cervix, such as during sex.
- Pain during sex.
- Vaginal discharge that is tinged with blood.
How Is Cervical Cancer Diagnosed?
As part of your regular pelvic exam, you should have a Pap test. During a Pap test, the doctor scrapes a small sample of cells from the surface of the cervix to look for cell changes. If a Pap test shows abnormal cell changes, your doctor may do other tests to look for precancerous or cancer cells on your cervix.
Your doctor may also do a Pap test and take a sample of tissue (biopsy) if you have symptoms of cervical cancer, such as bleeding after sex.
Sunrise Hospital offers comprehensive Cervical cancer treatment in Delhi encompassing advanced therapies such as surgery, chemotherapy, radiation, and targeted treatments. We have advanced technology and Cervical Cancer doctor in Delhi. All the Doctor are well experienced in their field and Get online and offline consultation.
How Is It Treated?
The treatment for most stages of cervical cancer includes:
- Surgery, such as a hysterectomy and removal of pelvic lymph nodes with or without removal of both ovaries and fallopian tubes.
- Chemotherapy.
- Radiation therapy.
Depending on how much the cancer has grown, you may have one or more treatments. And you may have a combination of treatments. If you have a hysterectomy, you won’t be able to have children. But a hysterectomy isn’t always needed, especially when cancer is found very early.
Cervical cancer found in its early stages can be successfully treated. The choice of treatment of Cervical Cancer and the long-term outcome (prognosis) of cervical cancer depend on the type and stage of cancer. Your age, overall health, quality of life, and desire to be able to have children must also be considered.
Prevention Of Cervical Cancer
You can treat early cervical cell changes (dysplasia), which can reduce your risk for cervical cancer. You can also reduce your risk for abnormal cell changes.
Get the HPV vaccine
If you are age 26 or younger, you can get the HPV vaccine. The vaccines Cervarix and Gardasil protect against two types of human papillomavirus (HPV) that cause cervical cancer. The series of shots is recommended for girls age 11 or 12 and can be given to females ages 9 to 26. You can get either vaccine.
Reduce your risk of a sexually transmitted infection (STI) Preventing an STI, including HPV, is easier than treating an infection after it occurs. HPV infection usually doesn’t cause symptoms, so you or your partner may not know that you are infected.
Have regular Pap test screening
The recommended Pap test schedule is based on your age and things that increase your risk. For most women, it is best to have a Pap test every 1 to 3 years. Talk to your doctor about when to have your first Pap test and how often to have this test.
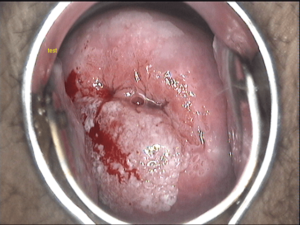
Colposcopic examination
Colposcopy is the current standard practice for early detection of Cervical Intraepithelial Neoplasia ( precursor cervical cancer ) in screen positive women.
At Sunrise, we offer colposcopic guided examination and cervical biopsy which can lead to early detection of cancer and with more accuracy. colposcopy can substantially reduce the number of blinded 4-quadrant cervical biopsies and unnecessary conizations and invasive surgical procedures for diagnosis.
In Delhi, adept Cervical Cancer specialist in Delhi provide expert care to patients. These experienced doctors possess a deep understanding of cervical cancer’s complexities, offering accurate diagnoses and tailored treatment plans. Sunrise Hospital is the Best place for Cervical cancer treatment in Delhi. We have one of the Best Cervical Cancer Doctor in Delhi. No compromise with treatment. The Cervical Cancer treatment cost in delhi depends on type of cancer.
FAQ 's
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry's standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged. It was popularised in the 1960s with the release of Letraset sheets containing Lorem Ipsum passages, and more recently with desktop publishing software like Aldus PageMaker including versions of Lorem Ipsum.
Sentinel Lymph Node Mapping
Sentinel lymph node mapping has the potential to decrease morbidity and optimize the pathologic assessment of identified nodes in women with endometrial cancer.
Accurate surgical staging is the most important prognostic factor in endometrial cancer, SLN mapping can be considered for the surgical staging of apparent uterine-confined malignancy when there is no metastasis demonstrated by imaging studies or no obvious extrauterine disease at exploration.
Sentinel lymph node (SLN) mapping, which has been used in other cancer types, may be an acceptable surgical strategy between a complete lymphadenectomy and no nodal evaluation in patients with endometrial cancer. SLN mapping is based on the concept that lymph node metastasis is the result of an orderly process; that is, lymph drains in a specific pattern away from the tumor, and therefore, if the SLN or first node is negative for metastasis, then the nodes after the SLN should also be negative. This approach can help patients avoid the side effects associated with a complete lymphadenectomy, Surgeon experience, adherence to an SLN algorithm, and the use of pathologic “ultrastaging” are key factors for successful SLN mapping.
At sunrise hospital we do SLN mapping for thorough staging , accurate prognosis and appropriate complete treatment. Cervical injection of Indocyanine green (ICG) for SLN Mapping that requires near-infrared camera for localization, provides a very high SLN detection rate.
Cervical Cancer – Surgery
Surgery to remove the cancer depends on the location and extent Treatment of cervical cancer and your desire to be able to have children. You also may be given radiation therapy, chemotherapy, or a combination of the two (chemoradiation). These treatments may be given before or after surgery to try to destroy any cancer cells that may remain or to help control or shrink the tumor.
Surgery choices
Surgery for very early stages of cervical cancer may preserve your ability to have children. Surgeries include:
- A cone biopsy or loop electrosurgical excision procedure (LEEP) . This removes a wedge of cervical tissue that contains the cancer.
- Radical trachelectomy . This removes the cervix, part of the vagina, and the pelvic lymph nodes (lymph node dissection). But the uterus is left in place.
Surgery for most stages of cervical cancer does not preserve your ability to have children. Surgeries include:
- Hysterectomy with or without removal of the ovaries. This removes the cervix and related organs where recurrence would be most likely.
- Modified radical hysterectomy with pelvic lymph node dissection. A radical hysterectomy usually includes removal of part of the vagina, the uterus, the ovaries, and the fallopian tubes. It removes the most likely sites of cancer and may reduce the risk of recurrence.
- At sunrise hospital we perform a laparoscopic encerclage with the radical Radical trachelectomy to avoid miscarriage in future pregnancies.
Dealing With Side Effects Of Surgery
Side effects from surgery can include difficulty with urination or problems with bowel habits, such as constipation or diarrhea. Your ability to have or enjoy sexual intercourse may also be affected.
Laparoscopic Treatment Of Cervical Cancer:
Today laparoscopic Radical Hysterectomy has become the standard of care for cancer cervix. The benefits of laparoscopy are maximal in these patients as there is complete removal of the cancerous tissue, Minimal blood loss, least damage to adjacent organ like bladder, bowel etc. and only 2-3 days hospital stay, minimal pain. Hence for Cancer surgery Laparoscopy has come as a boon as the quality of care is much superior the only challenge to this procedure is the surgeons expertise wherein ‘Sunrise provides the standardized treatment of Cervical Cancer. Specialist surgeon for cervical cancer treatment in delhi. Consul with experts.
Treatment Of Cervical Cancer
Treatment choices for cervical cancer may be a single therapy or a combination of therapies, such as:
- Surgery to remove the cancer. The type of surgery needed depends on the location and extent of cervical cancer and whether you want to have children.
- Chemotherapy, which uses medicines to kills cancer cells. It is usually used as the main treatment or after a hysterectomy. It may also be used along with radiation therapy.
- Radiation therapy, which uses high-dose X-rays or implants in the vaginal cavity to kill cancer cells. It is used for certain stages of cervical cancer. It is often is used in combination with surgery.
If you are looking for Treatment of Cervical Cancer. So Sunrise Hospital’s department performed safely cervical cancer surgery. Our commitment to patient well-being, coupled with their expertise, makes them invaluable assets in the fight against cervical cancer.
Sentinel lymph node (SLN) mapping, which has been used in other cancer types, may be an acceptable surgical strategy between a complete lymphadenectomy and no nodal evaluation in patients with endometrial cancer. SLN mapping is based on the concept that lymph node metastasis is the result of an orderly process; that is, lymph drains in a specific pattern away from the tumor, and therefore, if the SLN or first node is negative for metastasis, then the nodes after the SLN should also be negative. This approach can help patients avoid the side effects associated with a complete lymphadenectomy, Surgeon experience, adherence to an SLN algorithm, and the use of pathologic “ultrastaging” are key factors for successful SLN mapping.
At sunrise hospital we do SLN mapping for thorough staging , accurate prognosis and appropriate complete treatment. Cervical injection of Indocyanine green (ICG) for SLN Mapping that requires near-infrared camera for localization, provides a very high SLN detection rate.
In India, the best doctor for cervical cancer in India leads to renowned experts like Dr. Nikita Trehan. With a stellar reputation and vast experience in oncology, Who beacon of hope for those battling cervical cancer doctor in India. Known for their advanced treatment protocols and a patient-centric approach, they offer comprehensive care, from early diagnosis to personalized treatment plans, ensuring the best possible outcomes.
If you are looking for cervical specialist doctor in delhi, our hospital is the perfect place for treatment. Book online Appointment. World renowned best doctor for cervical cancer in India.
Team Of Specialists
Highly experienced team of super specialist now available at Sunrise Hospital